Virtually Fracture Free
Author: Paul Jenkins & Lech Rymaszewski
15/09/2017
We all have an image in our heads of fracture clinic waiting rooms, overcrowded and bursting at the seams, uncomfortable patients, wielding cumbersome white casts while they patiently wait......and wait.....
The digital age is upon us, and here in Glasgow, we have revolutionised the fracture clinic. Paul Jenkins and Lech Rymaszewski, two of the visionaries behind the Virtual Fracture Clinic, started in Glasgow and adopted worldwide, tell us how and why.....
Traditional # Clinics- The problem
The traditional fracture clinic model requires the patient to return the next day for review by an orthopaedic surgeon in a general clinic that could include any fracture throughout the body. Fractures were managed using casts and splints and were monitored for healing with repeated x-rays.
Many orthopaedic departments now manage “outpatient” trauma using a Virtual Fracture Clinic (VFC). Close co-operation with neighbouring Emergency Departments (EDs) and Minor Injuries Units (MIUs) is essential.
This demonstrates a year of patients with “outpatient” orthopaedic trauma that would normally be referred to a general fracture clinic. With the VFC only 41% required face-to-face review.
The Digital Age
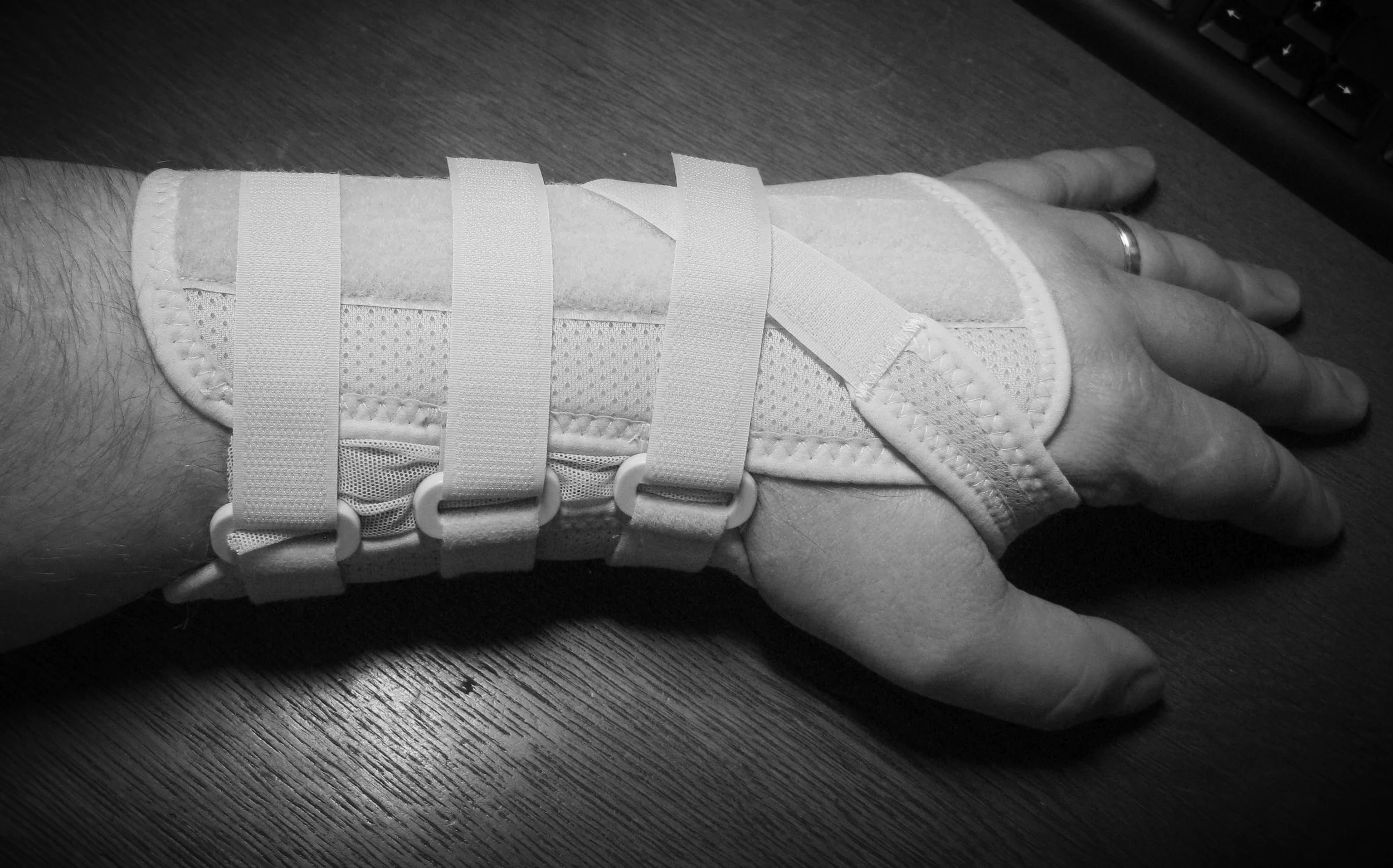
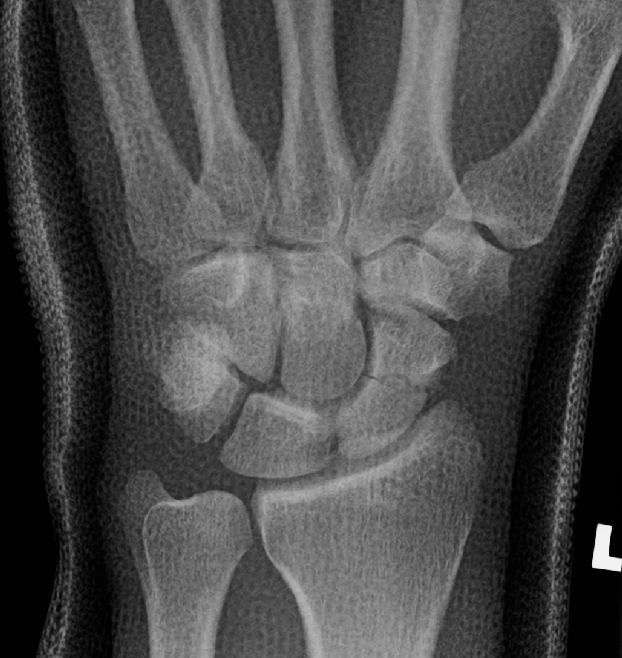
The resolution of x-rays and digital PACS systems has improved over time and images can be magnified and manipulated to the point where minor undisplaced cracks, of no consequence, are detected in increasing numbers. Evidence-based research has shown that many injuries, such as the occult radial head fracture (or Sail Sign) and paediatric wrist torus fractures are also injuries that heal best with a minimum of immobilisation. The introduction of removable splints for the wrist and ankle have reduced the need for cumbersome “backslab” plaster casts. These removable splints enable “self-care” as they can be removed by the patient for hygiene, promote early weight-bearing and be easily removed when healing has occured.
Generalist vs Specialist
Although a generalist can provide adequate care for most injuries, this leads to significant variation in treatment. It can also delay access to a specialist opinion when needed. The concept of a “general” orthopaedic surgeon has also been replaced with increased subspecialisation. The VFC allows effective triage of an injury to the most appropriate specialist for review at the most clinically suitable time; which is generally not the day after injury!
The VFC also harnesses the increased specialism and training of ED medical and nursing staff. Many patients with simple injuries are discharged with advice (backed up by information leaflets) and are not even referred to the VFC. It also utilises digital communication of x-rays and patients notes. There is now acceptance of contacting patients via telephone rather than a mandatory face-to-face review.
How does it actually work?
At the VFC the notes and x-rays of the patients seen the previous day, 7 days a week, are reviewed digitally by a consultant and a management plan is formulated. This is communicated to the patient, by a nurse, using the telephone. This can also be backed up by text, email and letter. Contemporaneous data is recorded in specialist forms in the electronic paper record, to facilitate comprehensive audit. Many patients are given advice over the telephone and don’t need to attend a face-to face appointment.
Only a small proportion need to come to hospital. For example, a patient with a proximal humerus fracture would be advised to come to the specialist shoulder fracture clinic a week later where an x-ray would be performed to check for secondary displacement. An unnecessary appointment the next day, when the patient was suffering their greatest pain, was therefore avoided.
Redesigned pathways can also be applied to many other common injuries such as the suspected scaphoid fracture; a common cause of referral from ED to fracture clinics. Modern imaging such as MR scans are increasingly available and cost-effective at the early diagnosis of these fractures. Doubt over diagnosis and prolonged immobilisation of simple soft-tissue injuries is avoided. The VFC manages this pathway, only bringing back those with definite fractures for review and treatment.
Benefits for all
The VFC has many benefits for the ED. Staff are empowered to use their training and skills to completely manage simple orthopaedic injuries that will heal well with simple symptomatic relief. The time spent in ED by a patient with an orthopaedic injury is reduced in the knowledge that the x-rays and history will be reviewed by a consultant orthopaedic surgeon the next day.
For the Orthopaedic Department, a reduction in the number of patients attending with trivial injuries allows adequate time for the management of complex injuries. It has also allow for the development of specialist elective services.
Spreading the news
The VFC model has been demonstrated to be safe, efficient and cost-effective. It was recognised with an national award in 2014 (HSJ Acute Sector Innovation). It has been adopted by many units in the UK and abroad that have recognised the clear benefits to patients and staff.
It has spread throughout the UK with departments either running a VFC (green) or in various stages of planning/implementation (other colours)
Patient Satisfaction
The VFC results in high patient satisfaction.
If you would like more information about how to set up a Virtual Fracture Clinic in your department, please contact Dr Paul Jenkins, Consultant Orthopedic Surgeon at Glasgow Royal Infirmary. Paul.Jenkins@ggc.scot.nhs.uk